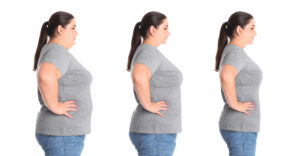
Obesity is linked to many serious health issues such as diabetes, cardiovascular disease and premature death, and the disease has reached epidemic levels.
Lifestyle changes such as exercising more and improving nutrition are important factors in controlling the disease, but for many patients it is not enough, and their doctor may recommend bariatric surgery. There are so many myths floating around regarding bariatric surgery that may scare you, so we will look at the five most common myths:
1. Bariatric surgery is a ‘cop-out’
Some people will think that doing bariatric surgery is a cop-out for those that are too lazy to do the work to lose weight – but once you fall into the morbidly obese category of a BMI of 35 or more it is extremely difficult to lose enough weight to protect your health. Patients will have to continue dietary and exercise guidelines to lose weight post-surgery as prescribed by their surgeon, but it should be easier. Obesity is not normally a choice, it is a disease that is often determined by metabolic, physiological, environmental and psychological factors or a combination thereof.
2. You will eventually regain the weight that you have lost
If you think that surgery is the magic bullet to a slim you, and you can eat anything you wish for whilst sitting on the couch post-surgery, you may very well regain the weight in the long term. It is the first step in a complete overhaul of your lifestyle and will require life-long commitment to compliance with better living guidelines.
However, most people continue to lose more weight and keep it off for twenty years or more after bariatric surgery. Patients who have undergone bariatric surgery have lower incidences of diabetes and cardiovascular disease, and mostly live longer.
3. You can’t get pregnant or have a healthy pregnancy after bariatric surgery
This common myth is completely unfounded. Obesity has been linked to infertility, and if you fall pregnant whilst obese, you have a much higher risk of developing medical problems during the pregnancy such as gestational diabetes, blood clots, pre-eclampsia, recurring infections and premature delivery.
Patients are advised not to fall pregnant for at least a year after bariatric surgery, because it interferes with the required weight loss, however, after this period it is in fact less of a risk to fall pregnant than when you were obese.
4. It is an elective procedure just to lose weight
Yes, in most cases it is an elective procedure, but not always, and it does carry some risks just like every other surgery, however, the risk of metabolic and other chronic diseases due to obesity far outweighs the risk of surgery if done according to best practice in a reputable facility.
Doubling your healthy weight increases your risk of dying ten times.
Health Awareness Facts Tweet
Obesity carries the risk of developing diabetes, cardiovascular disease, sleep apnoea, kidney diseases, joint problems and strokes. In contrast, bariatric surgery has shown encouraging results in many areas of health: a reduction of 50% or more of your excess weight in the first year, complete remission for many Type II diabetics, less joint problems and reduction in the severity of hypertension.
5. Post-surgery vitamin and mineral deficiencies can cause serious health problems
According to the American Society for Metabolic and Bariatric Surgery (ASMBS), bariatric surgery reduces absorption of nutrients from the intestine as well as a reduced intake of nutrients, which may lead to vitamin and mineral deficiencies. However, your physician will provide guidance and advice on nutritional compliance and regular follow ups should prevent any ill effects.
For those requiring bariatric surgery there are far more benefits than problems.